TAVI under conscious sedation – enabling continuity of treatment for your sAS patients
It remains essential that your severe aortic stenosis (sAS) patients continue to be referred for treatment, however many of them may be anxious about spending time in hospital and need a treatment that offers a shorter hospital stay and quicker return home. TAVI under conscious sedation can offer a range of benefits and address these patient needs.
Conscious sedation has benefits for patients vs. general anaesthesia1,4
TAVI has typically been performed under general anaesthesia, however in recent years there has been a pronounced switch towards the use of conscious sedation due to the range of advantages it may offer patients.1-3
For patients, conscious sedation:
- may help to relieve anxiety that they tend to feel with general anaesthesia4,5
- avoids the need of intubation that is normally required with general anaesthesia, which can help shorten their procedure time1,6
Conscious sedation is also generally considered a safe target state as ventilation is normally adequate and cardiovascular function is maintained (Figure 1).4,7
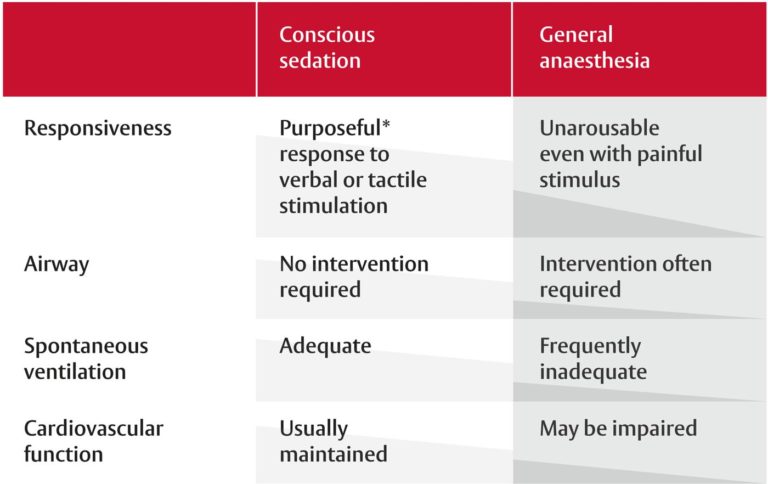
Figure 1 – Features of conscious sedation vs. general anaesthesia.7
With TAVI, your patients can receive an aortic valve replacement under conscious sedation
Unlike surgery, which can only be performed under general anaesthesia, TAVI under conscious sedation is an option for most patients.1,2,6
Conscious sedation has been used increasingly in TAVI procedures over time, with an increase from <2% in 2007 to ~70% of procedures in 2016 in the UK, and already around 50–75% of TAVI procedures in Europe between 2014 to 2016.2,6
Patients receiving TAVI with conscious sedation have demonstrated better outcomes compared to those who had TAVI with general anaesthesia, with significant improvements reported in mortality rates and quality of life.1,3,8

Figure 2 – TAVI outcomes with conscious sedation vs. with general anaesthesia.1,8
Further, TAVI under conscious sedation has also demonstrated shorter procedure times and shorter hospital stays compared to TAVI under general anaesthesia.1,3,8† This can help shorten waiting lists and opens the door to more of your patients being treated sooner.
As a result, TAVI can help reduce the impact on hospitals as well as reducing the costs normally associated with prolonged hospital procedures and stays.1,3,8
These benefits mean patients can come home quicker, with better outcomes and improvements in their overall quality of life.1,9,10
TAVI enables you to continue treating your sAS patients
TAVI can be a beneficial option for your patients compared to surgery, especially during times of concern when hospital systems are overloaded.3 In addition to shorter hospital stays, TAVI offers further benefits with the option of conscious sedation.1,3,8
It is important not to delay referring your patients. By continuing to refer patients for a TAVI evaluation, you can give them a fast, low-risk treatment and help reduce the burden on hospitals by reducing hospital and ICU stays.1,3,8
* Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
† Quality of life scores assessed using the Kansas City Cardiomyopathy 12-question survey.
Data based on observational studies, where potential selection biases in the absence of randomisation may be greater. Data should be interpreted with caution, as comparative effectiveness analyses using observational data cannot definitively establish the superiority of one technique to another.
Abbreviations:
sAS, severe aortic stenosis; TAVI, transcatheter aortic valve implantation; QoL, quality of life.
Check our latest articles
View all articlesReferences:
1 Villablanca PA, et al. Catheter Cardiovasc Interv. 2017; 1–13.
2 Ludman PF. Heart. 2019;105: s2–s5.
3 Hyman MC, et al. Circulation. 2017;136(22): 2132–2140.
4 Academy of Medical Royal Colleges. Safe Sedation Practice for Healthcare Procedures, October 2013.
5 Celik F, Edipoglu IS. Eur J Med Res. 2018;23: 41.
6 Sato K, Jones PM. J Thorac Dis. 2018;10(30): S3588–S3594
7
American Society of Anesthesiologists. Continuum of Depth of Sedation: Definition of General Anesthesia and Levels of Sedation/Analgesia, October 2019.
8 Toppen W, et al. PLoS ONE. 2017;12(4): e0173777.
9 Mack MJ, Leon MB. Two-year clinical and echocardiographic outcomes from the PARTNER 3 low-risk randomised trial. ACC 2020; Chicago, IL; March 28–30, 2020.
10 Baron SJ, Magnuson EA, Lu M, et al. J Am Coll Cardiol. 2019;74: 2833–2842.
Medical device for professional use. For a listing of indications, contraindications, precautions, warnings, and potential adverse events, please refer to the Instructions for Use (consult eifu.edwards.com where applicable).
PP--EU-0544 v2.0